Soft, Skin-Like Nasal Patch Could Transform Sleep Monitoring
May 14, 2026
By Tracie Troha
Sleep-related breathing disorders, including sleep apnea, affect millions of people worldwide but frequently go undiagnosed. One major barrier to diagnosis is the test itself.
Traditional sleep monitoring systems often rely on bulky equipment and nasal cannulas — small tubes inserted into the nostrils to measure airflow. While effective, these systems can be uncomfortable, intrusive, and difficult to tolerate overnight, limiting their use for long-term monitoring at home.
Now, researchers led by W. Hong Yeo, Peterson Professor in Pediatric Research at the George W. Woodruff School of Mechanical Engineering, have developed a soft, wireless nasal patch that could offer a more comfortable alternative for monitoring breathing during sleep.
The technology, described in a recent study published in Proceedings of the National Academy of Sciences (PNAS), uses ultrathin, skin-like wearable electronics to detect subtle movements of the nose caused by breathing without tubes, wires, or direct airflow measurements.
“This technology fundamentally improves the user experience by eliminating the primary source of discomfort: the insertion of prongs into the nasal airway,” Yeo said. “By utilizing an external, flexible patch that naturally conforms to the face, the device minimizes interference with both natural breathing and sleep posture.”
A New Approach to Sleep Respiration Monitoring
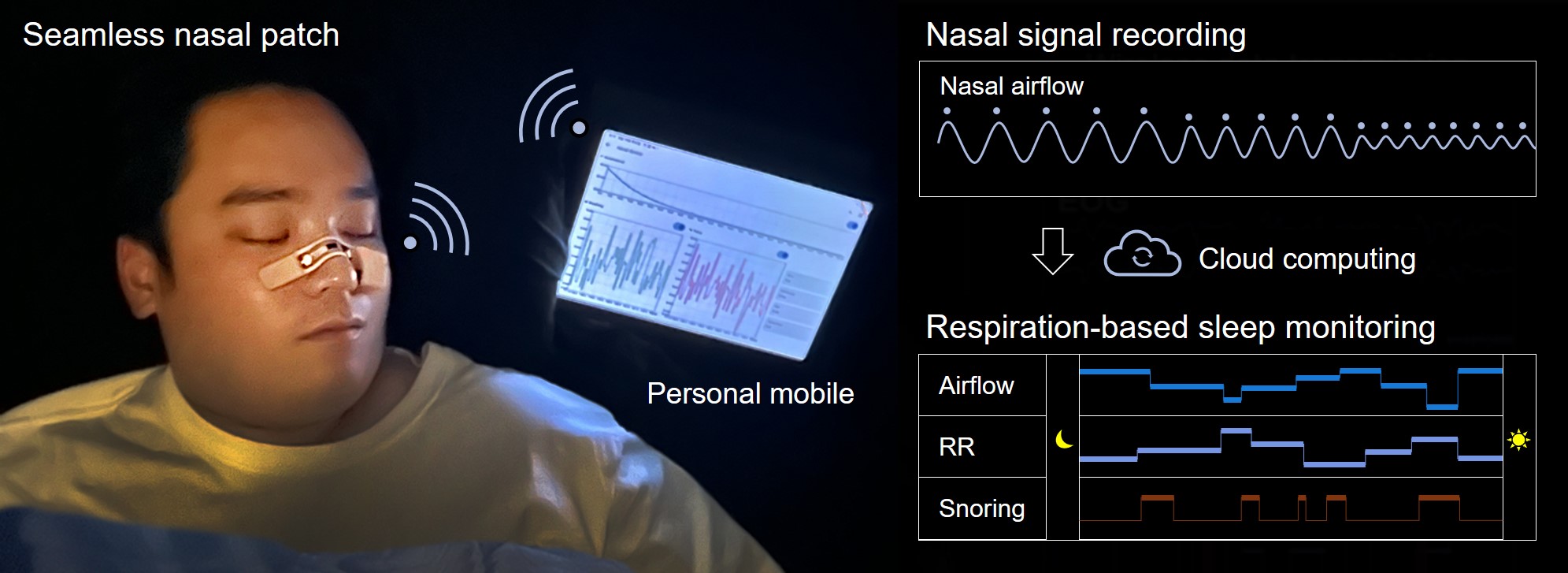
Instead of measuring airflow directly inside the nose, the patch senses tiny, natural stretching and movements of the skin around the nasal bridge caused by changes in breathing pressure.
The device adheres to the outside of the nose using a disposable medical-grade adhesive layer. Flexible strain sensors and wireless electronics embedded in the patch continuously collect respiratory data and transmit it to a mobile device in real time.
“It continuously tracks subtle tissue deformations and wirelessly transmits the respiratory data to a mobile device while the user sleeps, providing a completely non-invasive way to monitor breathing,” Yeo said.
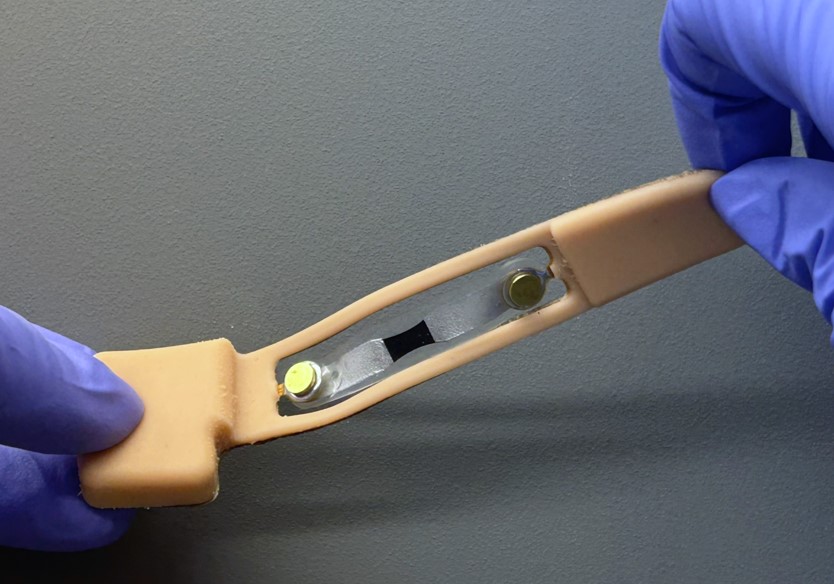
The patch also features a modular design that separates reusable electronics from disposable skin-contact materials, making it practical for repeated use.
Designed to Feel Like Skin
The central goal of the project was to create a device comfortable enough for long-term wear. Researchers built the patch to flex and stretch with the skin, allowing the sensor to maintain close contact with the nose without creating pressure or discomfort during sleep.
“Designing a skin-like device is critical for both user comfort and the accuracy of the sensor,” Yeo said. “It can conform perfectly to the curved surface of the nasal bridge and move seamlessly with the wearer.”
That flexibility also improves the device’s ability to capture accurate respiratory signals without losing contact or degrading performance overnight.
The team incorporated laser-induced graphene strain sensors and liquid-metal interconnects, soft conductive pathways that maintain stable electrical performance even during repeated movement and stretching.
Matching Traditional Monitoring Methods
In laboratory and overnight sleep studies, the patch produced results that closely matched those of conventional nasal cannula systems. Researchers found that the wearable device could reliably track normal breathing patterns, low-amplitude breathing, and even snoring events.
“What stands out most is how closely the patch’s performance mirrors traditional, invasive methods, despite being mounted entirely on the outside of the nose,” Yeo said.
The patch successfully reproduced respiratory waveforms over more than five hours of natural sleep and maintained stable performance without signal interruptions.
Expanding Access to Sleep Health
Researchers hope this technology could help make sleep monitoring more accessible, especially for patients reluctant to undergo traditional sleep studies.
“The primary motivation stems from the fact that sleep-related breathing disorders are highly prevalent but frequently go underdiagnosed due to the significant drawbacks of conventional monitoring technologies,” Yeo said.
Because the device wirelessly transmits data to mobile devices and cloud-based systems, the researchers also see potential for broader health applications, including long-term remote monitoring and earlier clinical intervention.
“The most exciting prospect is the ability to establish a fully integrated digital healthcare framework, allowing personalized medicine,” Yeo said. “Because the patch transmits data wirelessly to mobile devices, it opens the door for remote cloud-based storage, long-term continuous home monitoring, and ultimately, timely clinical interventions.”
The research also establishes broader design principles for future wearable health technologies that combine soft materials, wireless electronics, and physiological sensing into unobtrusive systems designed for everyday life.
In addition to Yeo, the research team included Jimin Lee, a postdoctoral research fellow in the Woodruff School; Hoon Yi, a former Woodruff School postdoctoral fellow; and Seong J. Cho, Byeongiun Lee, and Jungmin Kim from Chungnam National University in South Korea.

